All products are certified by dental expert Dr. Greg Grillo
Tooth extraction can be a strenuous process. Not only does it involve the removal of a tooth from its socket, but it also requires the disruption and rearrangement of your surrounding oral tissues.
The tooth extraction duration and following healing process puts strain on your entire body, not just your mouth. And after tooth extraction, the area around the extraction site is vulnerable to infection because of the disruption to its natural balance.
If you notice yellowish discharge coming out of the socket, this is a sign of an infection. Certain activities increase your risk of infection, but there are several treatment options depending on your situation.
This article tells you everything you need to know about infection after tooth extraction, including the symptoms, causes, and treatments.
How Common Is Infection After A Tooth Extraction? A Quick Look
Post-extraction infections around the gums and in the socket are relatively uncommon. Dry sockets - insufficient clotting on the extraction site - affect between two and five percent of all cases.
However, infection risk increases for certain patients, such as those with pre-existing conditions like diabetes or compromised immune systems. And if the extraction site is not properly cared for after surgery, infection risk increases as well.
One recent study shows that after wisdom teeth extraction, young people with strong immune systems have a 10% chance of infection. For those with immune system problems, that figure reaches 25%.
Signs Of Infection After Tooth Extraction
Most of the time, post-operative infections in your mouth won't go unnoticed.
There are several signs that the area of your extraction may be infected.
If you notice any of the following symptoms after a tooth extraction, seek medical attention:
1. Bad Breath That Doesn’t Go Away After Brushing
Bad breath is often one of the first indicators of post-operative infection.
For some, bad breath is genetic, caused by certain medications, or the result of poor oral hygiene. But if your bad breath lingers and doesn't improve with brushing, it may be a sign that something else is happening in your mouth.
Especially if you don't have a history of bad breath, there is a good chance this is a sign of infection.
2. Swelling, Redness, And Tenderness Near The Extraction Site
The area around your extraction site should look normal within three days of surgery. You might have an infection if it's just as swollen or red several days after the procedure.
Swelling is often accompanied by tenderness and redness, so keep an eye out for these signs as well. If the area around your extraction site is painful to touch and you notice it worsening, that's cause for concern.
3. Excess Oozing Or Yellow Discharge
Oozing and drainage from the extraction site are normal during the healing process. But if you notice more than usual or the fluid is thick and yellowish, your mouth is likely infected.
Usually, this discharge will be noticeable. It will smell bad and your mouth may feel worse than it did the day before.
4. Bitter Taste That Doesn’t Go Away After Salt Water Rinses
Rinsing with salt water is an excellent way to reduce inflammation and irrigate the area of your tooth extraction. Managing the pain from a tooth extraction by rinsing with salt water is usually successful.
When clearing your mouth with salt water, you also wash away any bacteria that may be present. A bitter taste that remains after rinses is usually the result of discharge or pus in your mouth, which usually tastes bad.
5. Fever And Flu-Like Symptoms
If your infection is severe enough, it can spread to other parts of your body. This is known as systemic infection. Systemic infections often lead to fever, chills, and a general feeling of illness.
You may also experience nausea and vomiting.
Sickness isn't an immediate sign of infection, though. After an invasive surgery like a tooth extraction, it isn't unusual for the pain and stress put on your body to cause a fever. Take your temperature, give yourself time to rest, and check for other signs before concluding that fever is a symptom of infection.
6. Pain That Doesn’t Respond To Prescribed Painkillers
After an extraction, your doctor or dentist will probably give you a prescription for a painkiller such as prescription-grade ibuprofen or a stronger drug. If your pain is too intense for regular pain meds to dull it, your extraction site might have opened itself up to bacteria growth.
It's worth noting that your mouth often needs time to heal and that pain is a normal part of the process. Ibuprofen isn't the strongest pain medication out there, so your pain could be due to general discomfort and low pain tolerance.
7. Temperature Sensitivity On Teeth
Millions of people have sensitive teeth. But if you aren't one of them, heightened sensitivity around your teeth and gums after an operation could indicate an infection is beginning to spread.
As the infection gets worse, the sensitivity will too. If you notice your teeth or gums are sensitive to heat and cold in a way they weren't before surgery, it's time to see your dentist as soon as possible.
8. Swollen Neck Glands (Lymph Nodes)
Your lymph nodes are small, bean-shaped glands that are spread throughout your body. Swollen lymph nodes usually indicate the presence of an infection, and swelling in the neck area could be a sign that your bad breath and other symptoms aren't due to poor oral hygiene but to a more serious issue.
Fever, cold, and flu can also cause your lymph nodes to swell, so additional symptoms should be present before concluding that your swollen glands are a sign of infection.
9. Pain Or Swelling Down Your Jawline
If you start to notice radiating pain or swelling down your jawline, you should visit your dentist or doctor immediately. This symptom can be an indication of infection in the area, which is usually caused by bacteria that have spread beyond the extraction site.
Especially if your lymph nodes are swollen or you have a high-degree fever, these symptoms can be a sign of a serious infection that requires medical attention.
10. Pain At Extraction Point Or Socket
Like some other symptoms of infection, pain at the extraction point is normal for a few days. Your mouth will take a while to heal, and you will experience at least slight pain or discomfort for a week or two.
But this pain should consistently be getting better. If it isn't improving after the first three to five days, you should investigate it further for possible infection.
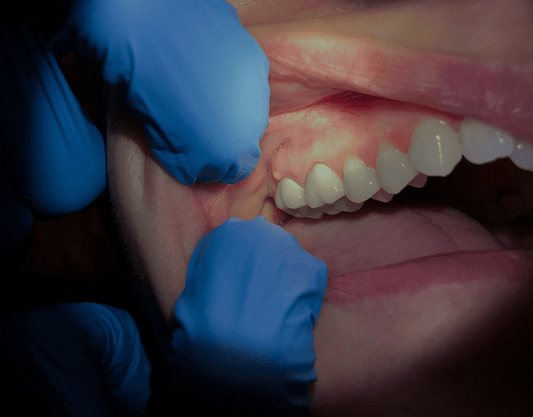
Tooth Extraction Infection Pictures
New infection starting to form after bottom tooth extraction.
Grey discoloration from a dry socket after tooth extraction.
Severe infection after an incisor (front tooth) extraction.
Treatments For Post-Extraction Infections
If you find out you have an infection, your next step will be to treat it. Depending on the severity, you'll have a few different options.
The good news is that most people will just need antibiotics and the infection should clear up in a couple of days. In more serious cases, you might need to have the abscess drained.
Below are the different treatments for post-extraction infections:
Additional Prescribed Antibiotics
Most dentists prescribe an antibiotic after tooth extraction on the day they complete the procedure. They will recommend you take the antibiotic for a certain number of days - usually five to seven - as a preventive measure.
If your dentist doesn't write you a prescription, you choose not to take it, or you take it and still develop an infection, your doctor or dentist will prescribe a stronger antibiotic.
Since most infections are noticeable after a few days at most, they don't have enough time to progress past the point where antibiotics can help. Usually, antibiotics are sufficient to clear up a post-extraction infection.
Abscess Drainage Or Removal
If the infection has progressed to an abscess, you may need to have it drained or removed. An abscess occurs when bacteria spreads in and around the extraction site and forms a pocket filled with pus.
This is usually done by your doctor using ultrasound-guided fine needle aspiration (FNA). This procedure involves inserting a very thin needle into the abscess and draining it of any accumulated pus.
Sometimes, your doctor will opt instead to perform surgery to remove the abscess. But this is usually only recommended if your infection is severe and easily accessible.
Saltwater Rinses
By drawing out excess fluid from your extraction site and surrounding tissues, saltwater rinses can sometimes help subdue your infection and provide temporary relief for an abscessed tooth. Salt also has disinfecting properties that can help clear out bacteria from your mouth.
To make a saltwater rinse, all you have to do is mix a one-quarter teaspoon of table salt with 8 ounces of warm water and swish it around in your mouth for 30 seconds before spitting it out.
You should do this three to four times daily until you have no more signs of infection.
Cold Compresses For Excessive Swelling Or Pain
A cold compress is often used to reduce inflammation and swelling in the face due to infection or trauma. The cold temperature constricts the blood vessels, decreasing circulation and reducing swelling or pain.
Unfortunately, they can't cure your infection on their own, but they can help you deal with the pain it causes.
To make a cold compress at home, wrap some crushed ice cubes in a thin towel and hold it against your cheek for 15 minutes at a time. If you don't have access to ice cubes, a bag of frozen vegetables can also do the trick.
Restricted Eating And Drinking
There are certain foods and drinks you should eat after tooth extraction, and the same applies if you have an infection.
Avoid any foods or drinks that are very hot in temperature, as this could aggravate the pain and swelling and slow down your healing process. Also stay away from eating anything crunchy and hard, as this could cause more trauma to the extraction site.
You should limit your consumption of sugary or acidic foods and drinks, as these can cause a spike in your blood sugar levels that could impede the healing process. And starchy foods like bread and chips might leave crumbs under the extraction site, worsening your infection.
If your infection is severe enough, you may need to stick to a liquid diet until it clears up. This will give your body time to heal without any additional strain or trauma from chewing hard food.
Bone Infection After A Tooth Extraction
Bone infections are rare compared to gum infections, but they are also more serious. If your doctor suspects a bone infection, they will usually take an X-ray to confirm the diagnosis and determine the extent of the damage.
The treatment for bone infections is similar to that of gum infections - antibiotics, salt water rinses, and occasional drainage - but there are some additional steps you may need to take.
If the infection is severe, your doctor may recommend surgery to remove any dead or infected tissue. This involves making a small incision to access the site, followed by cleaning and draining any necrotic (i.e., dead) material.
Your doctor may also recommend a bone graft, which will involve replacing any lost bone with a donor graft or an artificial substitute.
Tips To Avoid An Infection After Tooth Extraction
Tooth extraction costs a lot of money, requires significant recovery time, and can cause a lot of pain. Taking preventive measures to avoid infection ensures that your recovery time and costs are as low as possible.
Here are some tips you should follow to help reduce your risk of infection after a tooth extraction:
- Follow your dentist's post-extraction instructions carefully.
- Avoid drinking alcohol or smoking for at least 24 hours after the procedure.
- Don't rinse vigorously or use a straw for the first day.
- Avoid eating crunchy, hard foods that can get into the healing extraction site.
- Try to keep your mouth clean by brushing your teeth twice daily and flossing once daily (but don't apply too much pressure to the extraction site).
- Eat soft foods like mashed potatoes, yogurt, applesauce, and oatmeal for the first few days.
- Take ibuprofen or acetaminophen as recommended by your doctor to help manage pain and inflammation.
- Avoid hard exercise, heavy lifting, and extreme temperatures such as saunas or hot tubs, until your wound has healed completely.
The Bottom Line
Tooth extraction can be stressful, especially if your immune system is compromised.
Understanding the risk factors and taking preventive measures to reduce your chances of infection can help you have a more successful recovery.
If you experience any signs of an infection after tooth extraction, contact your dentist right away so they can start treatment as soon as possible. They will be able to provide you with the best advice and care for restoring your oral health.
Want to learn more? Here are some questions our customers frequently ask us.
What Does Gum Infection Look Like After Tooth Extraction?
Gum infection after tooth extraction may present as red, swollen gums near the extraction site. There may also be pus or a foul smell coming from the area. You may even notice the infected area in the mirror, but if it is deep in your gum tissue or on the upper jaw, you won't be able to see it.
How Long After Tooth Extraction Can You Get An Infection?
While infections can arise within 1-2 days post tooth extraction, you may not detect the signs of infection until 3-4 weeks later. It is important to pay attention to any indications that an infection has occurred following your dental procedure, even if your extraction site is healing without any complications.
How Do I Know If My Tooth Extraction Is Healing Properly?
If your tooth extraction is healing properly, you will notice your gums filling in around the extraction site and becoming less tender over time. Any pain or discomfort should decrease as the area heals, and there should be no visible signs of infection such as redness, swelling, or pus. If your ability to talk, chew, or swallow was impacted, you should also notice that your bite is shifting back to normal.
What Will A Dentist Do For An Infected Extraction Site?
Depending on the severity of your extraction, your dentist may recommend a variety of treatments to treat the infection. However, the typical process looks like this:
- Your dentist takes an x-ray to diagnose the situation.
- They prescribe an antibiotic to reduce the infection.
- Your dentist may then place a dressing on your extraction site to protect it while it heals.
- For more severe cases, your dentist may need to perform drainage to clean out the infected area.
What Color Is Infection After Tooth Extraction?
An infection after tooth extraction may present as red, swollen gums near the extraction site. In the case of dry sockets, you will notice a brown or grey discoloration around the afflicted area.
It is also common to see pus or a foul smell coming from the area. This pus will build up every few hours and ooze out or pop out of the socket. When this happens, you will see a yellowish-white or gray color from the extraction site.
Can An Infection After Tooth Extraction Spread To Other Parts Of The Body?
Yes, oral infections of any kind can spread to other parts of the body. If your infection goes untreated for too long, it can travel through your bloodstream and affect other areas of your body. In the vast majority of cases, the time between infection and treatment is not long enough for this to happen, however.
Will Infection Heal Itself After Tooth Extraction?
An infection will not heal itself after tooth extraction, as the infection-causing bacteria will remain in your gums unless it is properly treated. If left untreated, the infection may worsen, spread, and cause serious complications. It may also prevent your extraction site from healing properly.
Can Tooth Extraction Heal Without Antibiotics?
Antibiotics are standard protocol for treating an infection after tooth extraction, as they help your body fight off the infection-causing bacteria. Without antibiotics, the infection may spread or worsen and make it harder to treat in the future.
What Antibiotics Treat Tooth Extraction Infections?
Amoxicillin is the most common antibiotic used to treat infections after tooth extraction. Other antibiotics that might be recommended include cephalosporins and clindamycin, depending on the severity of your infection. In extreme cases, intravenous antibiotics may also be necessary.
Can Infection Remain After Tooth Extraction?
If your tooth is extracted due to a bone infection, the infection can remain after tooth extraction. This is rare, as the majority of infections after tooth extraction are limited to the soft tissues in your gums. Your dentist can prescribe you a strong antibiotic to treat any remaining infection.
Can smoking cause infection after tooth extraction?
The chemical toxins in cigarette smoke can make it more difficult for your body to heal an infection after tooth extraction. Smoking cigarettes is already a dangerous habit for your oral health, and smoking right after a tooth extraction can make it much more difficult for your body to fight off infection and heal the area.
Can Food Cause Infection After Tooth Extraction?
Certain foods can become lodged underneath your extraction site or irritate the area, which can lead to infection. You should avoid hard or crunchy foods like chips, bread, cereals, and nuts as well as any food that is hot and spicy. Sticking to a soft diet will help keep your extraction site clean and promote faster healing.
Can Infection Spread After Tooth Extraction?
Infection can spread to other parts of the body if it goes untreated for too long. First, it can spread to other parts of your mouth, like your teeth, jaws, or further down your gumline. It can also enter your bloodstream and spread to other organs in the body, although this is only a result of long-term untreated infection.