All products are certified by dental expert Dr. Greg Grillo
Newsflash: your teeth might have a much shorter lifespan than you. Dead teeth, also called necrotic, nonvital, or avulsed teeth, are a source of pain and discomfort. They are often the result of untreated decay or trauma to the tooth. When a dead tooth is present, it needs to be addressed immediately as it leads to further dental health problems such as infection and gum disease if left untreated. In this article, we will discuss what signs indicate you may have a dead tooth, treatment options for restoring your oral health, and ways to manage any associated pain while awaiting treatment.
Understanding A Dead Tooth: A Quick Look
A dead tooth, also known as a non-vital tooth, occurs when the delicate nerves and blood vessels inside the tooth's structure become compromised through damage or infection. This damage ultimately results in the tooth's pulp, the soft inner core containing nerves and blood vessels, dying. A dead tooth leads to both severe pain and potentially dangerous complications if left untreated, as it causes further infections, abscesses, and other oral health issues. In this comprehensive guide, we will thoroughly detail dead tooth symptoms, causes, and various treatment options, and share valuable prevention tips to help you maintain excellent oral health.
Recognizing Dead Tooth Symptoms
Persistent Bad Breath
A dead tooth causes relentless bad breath, often persisting even after rigorous brushing or using mouthwash. The primary reason for this symptom is the buildup of infection and decaying tissue deep within the tooth's structure, which emits a distinctly foul odor.
Unpleasant Taste In Your Mouth
An infected or dead tooth leads to a persistent and challenging-to-remove bad taste in your mouth. This unpleasant sensation frequently occurs as a result of the contaminated nerve tissue and fluids from the decaying tooth.
Swollen Gums Around The Dead Tooth
Swelling or inflammation in the gums surrounding the dead tooth is a significant symptom, which often signals an infection and the potential development of a dental abscess. The swelling may be visible near the base of the affected tooth, leading to redness and tenderness.
Tooth Discoloration
A dead tooth frequently undergoes discoloration, changing to a darker shade that ranges from yellow to brown or even black. This transformation is primarily due to the breakdown of blood cells, nerve tissue, and other internal components within the tooth's structure.
Pain In The Tooth Or Surrounding Gums
Experiencing pain in the tooth or the gums near the affected area may indicate the presence of a dead tooth. The intensity and persistence of pain vary widely and may worsen when consuming food, applying pressure to the tooth, or biting down, and sometimes even when the tooth is left undisturbed.
Tooth Sensitivity To External Stimuli
A dead tooth causes heightened sensitivity to heat, cold, or sweets. This symptom may become more pronounced when the tooth is exposed to cold water, air, or during the act of brushing, leading to a sharp or throbbing pain signal that there is a worrisome issue at hand.
What Causes A Tooth To Die?
To understand the underlying causes of a dead tooth, let's take a closer look at some of the key factors that could lead to a tooth dying.
Tooth Trauma
A tooth may die as a result of trauma or injury, which may occur due to a fall, a sports accident, or a physical altercation. When the blood vessels or nerves within the tooth become damaged, the tooth loses its ability to repair itself, eventually leading to its death.
Teeth Decay
Another leading cause of a dead tooth is untreated tooth decay. Over time, untreated tooth decay may progress deeper into the tooth, ultimately reaching the tooth's pulp. When this happens, the pulp becomes infected, and the tooth's nerves and blood vessels are severely affected, causing the tooth to die.
A Large Filling
Believe it or not, an extensive filling also contributes to the death of a tooth. Large fillings cause a tooth to become more vulnerable to bacterial invasion, causing inflammation and infection. In such cases, the tooth may lose its ability to fight off infection, ultimately leading to its death.
Dead Tooth Treatment Options
When faced with a dead tooth, it's important to consider the most appropriate treatment options. In this section, we'll discuss two common treatment methods for dead teeth: root canal therapy and tooth extraction.
Root Canal Therapy
A root canal is a widely-used and effective treatment for dead teeth; in fact, procedures are 98% effective. During a root canal, a dentist or endodontist will remove the infected tooth pulp, thoroughly clean the tooth canal, and then seal the tooth with a filling material to prevent further infection.
Dead Tooth Root Canal Before And After
Following a successful root canal treatment, a previously dead tooth should no longer show signs of infection or discoloration, and you should be pain-free. Additionally, the treated tooth will continue to function normally, allowing you to chew and bite comfortably.
Tooth Removal Or Extraction
In some situations, a dead tooth may be beyond saving, and a dentist may recommend the removal (extraction) of the tooth. This is typically done to prevent the spread of infection to neighboring teeth, the jawbone, or surrounding oral tissues. After the tooth is extracted, your dentist will discuss potential replacement options, such as dental implants, bridges, or partial dentures, to help restore your smile and maintain oral function.
Pain Management For Dead Teeth
Dealing with pain and discomfort associated with a dead tooth? Over-the-counter pain relievers and anti-inflammatory drugs may provide temporary relief to manage the pain. Popular choices include ibuprofen, acetaminophen, and aspirin. However, it's essential to remember that using pain medication should not be relied upon as a long-term solution, as the root cause of the issue needs to be appropriately addressed by a dental professional.
Essential Tips For Preventing Dead Teeth
To minimize the risk of developing a dead tooth, it's crucial to adopt healthy lifestyle habits and prioritize dental hygiene. Here are a few key tips to bear in mind:
Schedule Dental Visits At Least Once A Year
Scheduling regular dental checkups, preferably twice a year, are an effective way to detect and treat any potential oral health issues before they escalate into more significant problems. During these visits, your dentist will assess your teeth and gums, perform a thorough cleaning, and recommend any necessary treatments.
Maintain A Healthy Diet For Optimal Tooth Health
Consuming a well-balanced diet that is low in sugar helps maintain healthy teeth and gums. Foods rich in vitamins and minerals, such as calcium and phosphorus, contribute to robust and cavity-resistant teeth. Including fresh fruits, vegetables, whole grains, and lean proteins in your diet contribute to better oral health.
Drink Water For Overall Oral Health
Drinking water regularly throughout the day helps rinse away food debris, prevents the occurrence of dry mouth, and promotes saliva production. Saliva is essential for neutralizing acids and maintaining a balance of good and harmful bacteria in the mouth. Staying well-hydrated reduces the risk of developing tooth decay, gum disease, and other oral health issues.
In conclusion, adopting these preventive measures and maintaining a consistently healthy dental routine will significantly lower your risk of experiencing a dead tooth or other severe dental concerns. Don't forget the importance of consulting a dental professional for proper guidance and treatment options when necessary.
Wear A Mouthguard To Protect Your Teeth
Wearing a mouthguard during sports, recreational activities, or any other activities that could potentially result in injury to your teeth is a great preventative measure. A well-fitted mouthguard helps protect your teeth from impact and minimizes the risk of chipping, cracks, or other damage that may lead to a dead tooth.
Maintain Good Oral Hygiene For A Healthy Smile
One of the most important factors in preventing dead teeth is practicing proper oral care. This includes brushing your teeth for two minutes at least twice a day, flossing daily to remove plaque and food particles from between your teeth, and using mouthwash as needed to help kill bacteria and freshen your breath.
Additionally, maintaining regular dental checkups and cleanings with your dentist every six months will aid in the detection and prevention of dental problems. If all that is tough to remember, don’t worry: the CDC offers a comprehensive list of what a good oral hygiene routine looks like.
How Long Can A Dead Tooth Stay In Your Mouth?
A dead tooth, also known as a nonvital tooth, should be addressed and treated by a dental professional as soon as it is discovered. Although there is no fixed timeline for how long a dead tooth can stay in your mouth without causing complications, dealing with it promptly helps prevent issues such as oral infection, abscesses, and tooth loss.
Leaving a dead tooth untreated in your mouth leads to further dental problems, including damage to the surrounding teeth, gums, and even bone. In severe cases, an untreated dead tooth results in the spread of infection to other parts of your body and has detrimental effects on your overall health. Therefore, it is crucial to seek dental care as soon as you suspect that you have a dead tooth to ensure that it is treated effectively and to minimize any potential risks.
Whether you have a black dot on your tooth or you're concerned about the presence of a dead tooth, don't hesitate to seek professional dental advice. Practicing good oral hygiene and taking preventative measures go a long way in maintaining a healthy smile, but visiting a dentist for regular checkups and when problems arise is essential in ensuring optimal dental health.
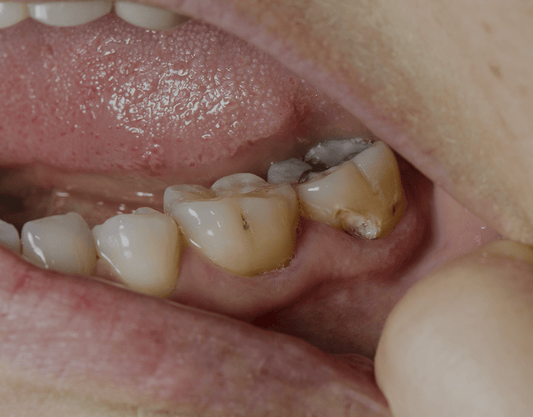
What Does A Dead Tooth Look Like?
A dead tooth, also known as a non-vital tooth or a necrotic tooth, typically presents noticeable discoloration. These changes in appearance manifest as a range of colors, including shades of yellow, brown, grey, or, in more severe cases, black. Aside from the discoloration, you may observe visible signs of decay, cracks, or structural damage to the affected tooth. It's essential to monitor your oral health and consult a dental professional if you suspect you may have a dead tooth.
Can A Dead Tooth Kill You?
While a dead tooth, in and of itself, is not directly fatal or life-threatening, the issue may morph into a more severe problem if left untreated. In some cases, a dead tooth leads to an infection in the gums, jawbone, or even the surrounding teeth. If the infection spreads further into the bloodstream, it results in a systemic infection called sepsis, which is potentially life-threatening. In rare instances, an untreated infection from a dead tooth could migrate into the brain, causing abscess formation or meningitis – both of which are hazardous if not addressed promptly. In summary, while a dead tooth won't kill you outright, neglecting to treat it leads to severe health complications.
Will A Dead Tooth Fall Out?
A dead tooth will not necessarily fall out on its own. Instead, the primary concern related to a dead tooth is the possibility of infection or decay that may result from the tooth's compromised state. Left untreated, the infection or decay spreads to other teeth or affects the supporting structures, including bone and gum tissue. This deterioration of the tooth's support system leads to eventual tooth loss. However, this outcome may vary depending on the individual case and the overall condition of the affected tooth. To prevent tooth loss or further complications, it's crucial to consult with a dentist promptly and follow their treatment recommendations to address the situation effectively.
How To Whiten A Dead Tooth
When it comes to whitening a dead tooth, traditional teeth whitening methods like over-the-counter products and at-home treatments are not effective, as these are designed for live teeth with surface stains. Instead, other dental procedures help restore the normal appearance of a dead tooth.
-
Internal Bleaching: One such procedure is internal bleaching, a treatment that whitens the tooth from the inside by placing a bleaching agent within the tooth itself. The dentist will first perform a root canal treatment to remove any infected material, clean the inside of the tooth, and then fill the tooth with a temporary material before sealing it. The bleaching agent will be applied several times over multiple visits until the desired shade is achieved, after which the tooth will be permanently sealed.
-
Dental Veneers: Another option for addressing the discoloration of a dead tooth is the application of dental veneers. These thin, custom-made shells, typically made of porcelain or composite material, are designed to match your surrounding teeth and are bonded to the tooth's surface, providing a natural-looking and long-lasting solution.
- Crowns: In more severe cases or when the tooth structure has been compromised, a crown may be recommended. Crowns are custom-made tooth-shaped caps that cover the entirety of the discolored tooth and offer both cosmetic and structural benefits. This treatment helps to preserve the remaining tooth structure, while also improving the overall appearance of the tooth.
Can A Dead Tooth Be Saved?
In many cases, a dead tooth is saved, especially if the tooth's structure remains intact and a dentist addresses the infection promptly. The most common treatment for saving a dead tooth is root canal therapy, during which the dentist will remove the infected tissue, clean the inside of the tooth, and then fill and seal the tooth with a biocompatible material. This procedure successfully preserves the tooth and prevents further issues, such as abscess formation or the spread of infection.
Does A Dead Tooth Need To Be Removed?
Not every dead tooth necessitates removal, and as mentioned earlier, root canal treatment often saves the tooth if caught early on. However, there are situations where extraction may be necessary. These scenarios typically include:
- In cases where the tooth cannot be saved through root canal treatment due to extensive damage to the tooth structure or surrounding bone
- When the infection has spread beyond the tooth and caused a more severe issue, such as a dental abscess or periodontal disease
- If the patient suffers from a compromised immune system, making it difficult to control the spread of infection
It's important to remember that prompt dental care is key to avoiding extraction and successfully treating a dead tooth. If you suspect you may have a dead tooth, don't hesitate to consult your dental professional for evaluation and guidance.
Is It Possible To Live with A Dead Tooth?
Although it is possible to live with a dead tooth for a limited period, it is strongly recommended not to leave it untreated. Failing to address the issue results in further complications, including infection, the formation of abscesses, and ultimately, tooth loss.
The Importance Of Dental Consultation For A Dead Tooth
Obtaining a dental consultation and proper treatment is crucial for managing dead teeth. Your dentist assesses the condition and recommends the most suitable treatment options, thereby minimizing the risks of complications associated with dead teeth.
The Lifespan Of Dead Teeth
The lifespan of a dead tooth primarily depends on the kind of treatment it receives. Properly treated dead teeth potentially last for numerous years, but neglecting their treatment could lead to further damage and, ultimately, the loss of the affected tooth.
How Dental Treatment Affects The Life Of A Dead Tooth
Several treatment options, such as root canal therapy or tooth extraction, extend the life of a dead tooth. The appropriate therapy prevents the spread of decay or infection to neighboring teeth and the jawbone, ensuring better overall dental health.
Identifying Pain In A Dead Tooth
A dead tooth indeed causes pain, and this discomfort stems from various factors like infection, inflammation, or pressure exerted while biting and chewing.
Symptoms Associated With The Pain In A Dead Tooth
Depending on the cause of the pain, individuals may experience symptoms such as throbbing, sensitivity, or dull aches. Furthermore, the intensity of the pain varies from mild to severe, with some cases requiring immediate professional attention to alleviate this discomfort.
Is A Dead Tooth Weak?
A dead tooth indeed becomes weaker over time due to several contributing factors. These factors include structural damage, decay, or the loss of vitality in the tooth's pulp. It is important to note that a weakened tooth may be more susceptible to breaking or fracturing, which leads to additional dental problems.
When a tooth loses its vitality, it no longer receives blood flow and essential nutrients from the pulp, which is the soft inner tissue responsible for a tooth's overall health. As a result, the tooth structure becomes compromised and progressively weaker.
Can A Dead Tooth Get Infected?
Yes, a dead tooth is prone to infection as the pulp inside the tooth loses its vitality and becomes a breeding ground for bacteria. This bacterial growth leads to the formation of an abscess—a pocket filled with pus and infection.
If left untreated, an infected dead tooth causes significant discomfort and swelling, and may even spread the infection to surrounding tissues and other parts of your body, potentially causing serious health complications. Check this list of symptoms to see if your tooth infection may be spreading throughout your body.
Are Dead Teeth Common?
Dead teeth are not necessarily a rare occurrence, and various factors, such as trauma or tooth decay, lead to a tooth's death. Injuries, such as a hard knock to the tooth, damage blood vessels within the pulp, causing the tooth to lose its vitality.
Tooth decay, on the other hand, results from poor dental hygiene, excessive sugary diets, or various dental conditions, leading to the destruction of tooth enamel and dentin, eventually reaching the pulp and causing a tooth's death.
Can A Dead Tooth Make You Sick?
An untreated dead tooth indeed poses a risk to your overall health. As mentioned earlier, a dead tooth is susceptible to infection, which subsequently spreads to other parts of your body, making you sick. In some cases, these infections lead to serious complications, such as sepsis, which are life-threatening.
Therefore, timely dental intervention and proper management of a dead tooth are crucial to prevent infections and maintain overall well-being.
Why Does A Dead Tooth Turn Black?
A dead tooth turns black due to the breakdown of blood cells and pulp tissue within the tooth, which leads to the characteristic dark discoloration. It is important to note that blackened teeth also result from other factors, such as the consumption of certain foods and beverages or smoking. However, a black tooth is alarming and must be assessed by a dental professional to determine the root cause and implement appropriate treatment if necessary.
By understanding the symptoms, causes, and treatments of a dead tooth, as well as taking preventive measures, you will maintain optimal oral health. Regular dental visits and good oral hygiene practices, such as brushing twice a day, flossing daily, and using fluoride-containing products, are crucial in avoiding dead teeth and promoting a healthy smile.
So What’s The Deal With Dead Teeth?
Dead teeth are the result of a variety of causes and lead to serious complications if left untreated. It is important to recognize the signs of a dead tooth so that it is adequately treated to prevent further damage and potential pain. Treatment for a dead tooth may involve root canal therapy, extraction, or other restorative treatments. If you suspect you have a dead tooth, contact your dentist immediately for diagnosis and treatment options. With proper care and attention, it’s possible to address any issues related to dead teeth so that they don’t cause long-term problems down the line.