All products are certified by dental expert Dr. Greg Grillo
Think of the resorption of teeth like a cavity that is eating away at your entire tooth - literally. It’s a condition that affects 5 to 10% of the general population who have never done orthodontic treatment.
If you’re concerned that you may be experiencing resorption, this article is for you. We’ll discuss the causes, symptoms, and treatment options for the resorption of teeth so you can start to improve your smile.
What Is Dental Resorption? - An Overview
Resorption of teeth is a process whereby the outer layer of a tooth - the enamel - erodes away, leaving the underlying layer of dentin exposed. It’s an incredibly serious dental problem that can cause pain, increased sensitivity to hot and cold temperatures, discoloration of the affected tooth, and even tooth loss if left untreated.
In dental terms, the process of resorption is the dissolution or breakdown of tooth structure. This can be inflammation and loss of dentin (the tissue under the enamel) or cementum (the outer parts covering the roots of the teeth).
Resorptive lesions generally start in the crown portion of a tooth, but they can also spread to other parts.
Resorption happens when your body rejects the tooth as a self-defense mechanism. There are many factors that can cause resorption, including genetics, trauma or injury to the mouth, hormonal changes during pregnancy or menopause, gum disease, and other infections.
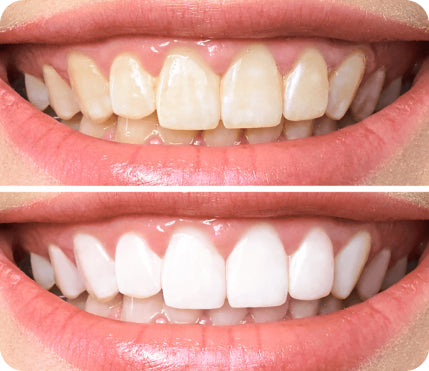
Root Resorption Before And After
Types Of Dental Resorption
There are two primary types of dental resorption: external and internal. What’s the difference? Let’s find out.
Internal Tooth Resorption
Internal tooth resorption is the more uncommon type of dental resorption. It occurs when cells inside the tooth begin to break down and erode away, leaving a hole in the center of the affected teeth. Having a hole in the center of your teeth is certainly a cause for concern, as you are more susceptible to decay.
You’ll know when you have internal resorption because the affected tooth will be sensitive to both hot and cold temperatures, as well as sweet foods. The tooth may also be prone to chipping and have holes that aren’t cavities. The area may feel different than other teeth when you press on it with your tongue or finger and can have a reddish tint to it.
External Tooth Resorption
External tooth resorption is much more common and happens when the outer layer of enamel erodes away, leaving the underlying dentin exposed. This can be caused by trauma or injury to the mouth, as well as gum disease.
The symptoms of external tooth resorption are similar to those of internal resorption - and can even occur concurrently with internal resorption. In addition, there may be small pits on the surface of the teeth. Because of this, it’s often difficult to diagnose external resorption.
What Causes Resorption?
The most common cause of resorption is trauma or injury to the mouth, either through a physical blow or during dental work. Although genetics is often mentioned as a cause, there is no consistent scientific evidence to prove this.
Other causes may include:
- Hormonal changes - Changes in hormones can lead to an increase in acidity levels in the mouth, making teeth more vulnerable to resorption. This is especially true for women who experience hormonal shifts due to pregnancy or menopause.
- Gum disease - Certain forms of gum disease can lead to the destruction of tooth structure, making teeth more vulnerable to resorption.
- Infections - Bacterial infections in the mouth can weaken the enamel and contribute to resorption.
- Untreated cavity - When cavities are left untreated, swelling, and infection can occur in the surrounding tissue, leading to resorption.
- Prolonged use of orthodontic treatments - Prolonged use of braces or other orthodontic treatments can cause pressure on the teeth, resulting in resorption.
Complications From Resorption
Resorption of teeth can cause several complications that get worse over time. These include:
- Pain - The exposed dentin layer is much more sensitive to heat and cold temperatures than the enamel, leading to increased pain and sensitivity.
- Discoloration - The dentin layer beneath the enamel is yellow in color, so when it’s exposed by resorption, you’ll likely see discoloration of the affected tooth.
- Tooth loss - In severe cases, tooth loss may occur if the resorption process continues without interruption.
- Infection - An exposed dentin layer is more vulnerable to infection, which can result in further issues.
- Crooked and chipped teeth - Because the enamel is eroded away, teeth may become misaligned or chipped.
- Cavity-like holes - Occasionally, resorption can cause cavity-like holes to form in the teeth.
Resorption Vs. Reabsorption: What’s The Difference?
Resorption and reabsorption are two similar-sounding words, but they have very different meanings when it comes to dentistry. Resorption is the process we’re focusing on in this article, in which the enamel is eroded away by acids or bacteria. Reabsorption, on the other hand, refers to the body’s natural ability to absorb minerals from food and beverages that can help rebuild weakened teeth.
What Are The Symptoms Of Dental Resorption?
It could be argued that complications that show up from dental resorption are also signs. The most common indications of resorption include:
- Pain when eating or drinking hot, cold, acidic, or sweet foods and beverages
- Increased sensitivity of the affected tooth/teeth
- Discoloration, which may be yellow, brown, or black in color
- Loss of enamel on the surface of the tooth
- Cracks or fractures in the affected teeth
- Pink or dark spots on the teeth
- Shifting teeth
- Swelling and red gums
If you notice any of these symptoms, contact your dentist right away so they can diagnose and treat the issue before it gets worse.
Treatment For Dental Resorption
Thankfully, there are multiple tooth resorption treatment options available.
Depending on the severity of the erosion, your dentist may recommend one or more of the following treatments:
Surface Dentine Treatment
If you’re lucky enough to catch the resorption early, surface dentine treatment may be an option. This treatment is used when there is mild to moderate resorption on the surface of the tooth. It involves applying a sealant or bonding material to the affected teeth in order to stop more damage from occurring and strengthen the teeth again.
Root Canal
Root canal therapy is a common treatment for internal dental resorption. During this procedure, your dentist will remove the infected pulp from inside the affected tooth and fill it with an inert material to protect against further damage. This can help to protect the remaining healthy tissue from further damage and allow for a complete restoration of the tooth.
Crowns
Using crowns differs from root canal therapy in that it won't help treat the infection. Instead, it may be necessary to protect the weakened tooth from further damage and restore its structural integrity. If the tooth isn't strong enough to support a crown, your dentist may recommend an implant.
Gum Surgery
When it comes to more urgent cases, gum surgery may be necessary to treat the infection and stop it from spreading. The procedure involves removing infected tissue or bone, cleaning the area, and then closing any gaps with stitches.
Tooth Removal (Extraction)
With extraction, your dentist will remove the affected teeth. This is usually done as a last resort and only when all other treatment options have been exhausted. Removal will ensure that the infection doesn’t spread to other teeth and also relieve any pain or discomfort caused by the resorption.
For more information about dental resorption, read on for some frequently asked questions.
Can Teeth Whitening Cause Resorption?
Cervical root resorption can result from internal bleaching if the procedure isn’t done properly or the surrounding tooth structure isn’t protected. For external bleaching, it’s recommended not to use concentrations of carbamide peroxide higher than 10%.
It is rare that teeth whitening would cause resorption, but if you have gum disease or any other dental infections, it may be best to postpone any whitening treatment until after they are treated.
How Common Is Root Resorption With Invisalign?
Root resorption is not a common side effect of Invisalign, but it is always a possibility. A study showed that the potential root resorption rate is just <10% of the original root length, meaning that it is a very rare occurrence.
Can Retainers Cause Root Resorption?
Retainers can cause root resorption if they are worn too long or too often, as this can put excessive force on the teeth and roots. If you are wearing a retainer, it is important to follow your dentist’s instructions for how often to wear it and how long each day.
How Common Is Root Resorption After Braces?
Root resorption following braces is uncommon but possible. If it does occur, studies show that wearing braces isn’t often the direct cause, and root resorption typically stops after braces are removed. The risk can be reduced by having regular check-ups and using bracket systems with low force levels during the course of treatment.
How Long Can A Tooth With Resorption Last?
The length of time a tooth with resorption can last depends on the severity of the condition and how well it is treated. If it isn’t treated, advanced stages of resorption can lead to tooth loss. But if caught early, treatment may be able to halt or even reverse the process and preserve your natural teeth for a longer time.
How Do You Heal Tooth Resorption?
The most crucial step to healing tooth resorption is to visit a dentist as soon as you notice any symptoms. Depending on the severity of your condition, they may recommend treatment such as root canal therapy, fillings, or crowns. In some situations, medication may be prescribed to reduce inflammation and discomfort.
Can Tooth Resorption Spread To Other Teeth?
Yes, tooth resorption can spread to other teeth if left untreated. The way this happens is that bacteria in the mouth can find their way into the affected tooth, leading to an infection. This infection can then spread to other teeth if it is not treated promptly. In one study concerning children and adolescents, root resorption of at least one adjacent tooth was found in two-thirds of the sample.
Can Stress Cause Tooth Resorption?
Stress is not a direct cause of tooth resorption, but it can increase your risk of developing the condition. Stress has been linked to increased production of certain hormones that can weaken the tissues around the teeth, leading to damage and eventual resorption.
It might be a surprise that stress can have effects on oral health, but adopting healthy lifestyle habits such as exercise and relaxation techniques can help you keep your dental health in good shape.
What Happens If You Don’t Treat Tooth Resorption?
If tooth resorption is left untreated, it can cause the affected tooth to become brittle and eventually break. In addition, it increases your risk of developing an infection in the root canal or gum tissue around the affected tooth. Therefore, if you suspect you have resorptive lesions on your teeth, you need to seek treatment from a professional as soon as possible.
Can You Prevent Bone Resorption?
There are several steps you can take to prevent bone resorption around your teeth. By taking good care of your oral hygiene (brushing and flossing daily) and visiting the dentist regularly for check-ups and cleanings, you can help protect against bone loss due to gum disease or other factors. Eating a balanced diet rich in calcium is also vital for preserving healthy bones in the jaw.
How Common Is Tooth Resorption In Adults?
Tooth resorption is rare in adults, but it does occur. As stated previously, it’s a condition that is present in 5 to 10% of the general population who has never had orthodontic treatment. The most common cause of tooth resorption in adults is periodontal disease or a traumatic injury to the teeth. Other causes include tumors, medications, and systemic diseases that affect dental structures.
Is Tooth Resorption Related To Osteoporosis?
Osteoporosis is a medical condition that weakens bones and can lead to fractures or breaks. Tooth resorption can be related to osteoporosis when resorption happens to the jawbone, as it affects the periodontal tissues and natural structures in the mouth.
Does Vitamin D Increase Bone Resorption?
Interestingly, vitamin D is known to help prevent bone resorption by increasing calcium absorption in the intestines and raising serum calcium levels. Adequate vitamin D levels can help build and maintain strong bones, so ensure you get enough from your diet or supplements.
How Fast Can Root Resorption Happen?
Root resorption can occur over a period of months or even years. This is why regular dental check-ups are key - it allows your dentist to identify any changes that may be occurring and take steps to prevent further damage from happening.
Is Resorption An Infection?
No, resorption is not an infection. It is a process in which the body breaks down the hard tissues of teeth and bones due to physical trauma or disease. However, infections can be one of the factors that lead to resorption.
What Disease Increases Bone Resorption?
Periodontitis, or advanced gum disease, is a common cause of bone resorption. This occurs when bacteria in the mouth infect and destroy the gums and surrounding tissues, leading to bone loss around the teeth. Other diseases may include arthritis, osteoporosis, cancer, and diabetes.
What Stimulates Bone Resorption?
Bone resorption can be caused by physical trauma, such as grinding or clenching your teeth or periodontal disease. Other factors that can contribute to bone resorption include systemic diseases (such as diabetes and osteoporosis), genetic disorders, and certain medications.
Does Tooth Resorption Cause Pain?
Yes, tooth resorption can cause pain. When the body breaks down the hard tissues of teeth and bones, it can cause an increase in sensitivity to hot or cold foods and drinks. On a deeper level, the process can cause pain in the jaw or neck, as well as discomfort when chewing. As the resorption process advances, the pain can become more severe.
Wrapping Up
Resorption is not a condition to be taken lightly. For those concerned about possibly suffering from resorption, x-rays, and other diagnostics can help diagnose the condition and determine the best course of treatment.
No matter whether you have internal or external resorption or whether it’s caused by trauma, genetics, infection or something else, there are plenty of treatment options available to help protect and restore your teeth.
If you’re experiencing any of the symptoms discussed in this article, it’s important to get in touch with a dentist right away. With prompt treatment, it is possible to stop resorption and preserve your teeth for many years to come!